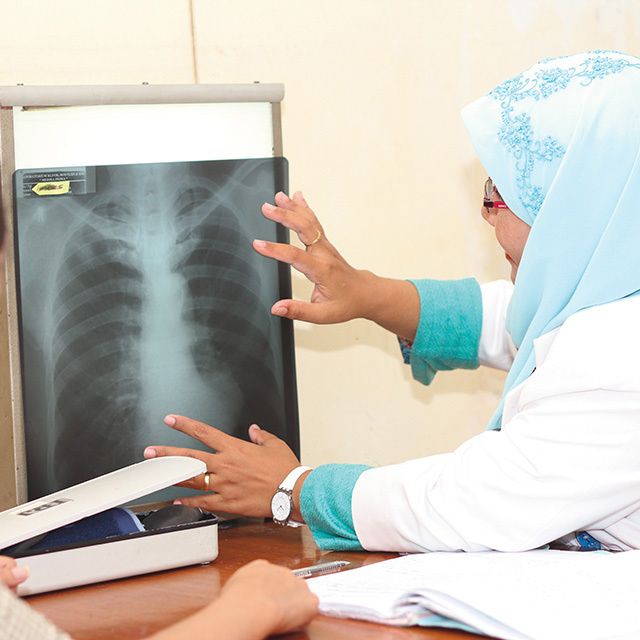
Previously, surgeons only had their individual skills to rely on. Now that has been transformed by advanced technology in the surgical theater: teamwork is led by Japanese medical science and middleware technology to improve safety.
SCOT is an advanced system that integrates an open MRI scanner and a surgical navigation system with other medical devices used during surgery, such as a rapid diagnostic test system, a 4K3D microscope monitor, and a surgeon’s cockpit. A prototype was constructed in 2016. In 2019, Hyper SCOT, the newest version, designed to incorporate advances in robotics and AI, became available for clinical research at Tokyo Women’s Medical University. The staff there was the first to use the newly integrated system to conduct brain surgery, with successful results that confirm the value of the approach. Since then, use of Hyper SCOT has steadily been increased within clinical research, including 46 neurosurgical procedures, mostly to treat brain tumors (as of April 8, 2020).
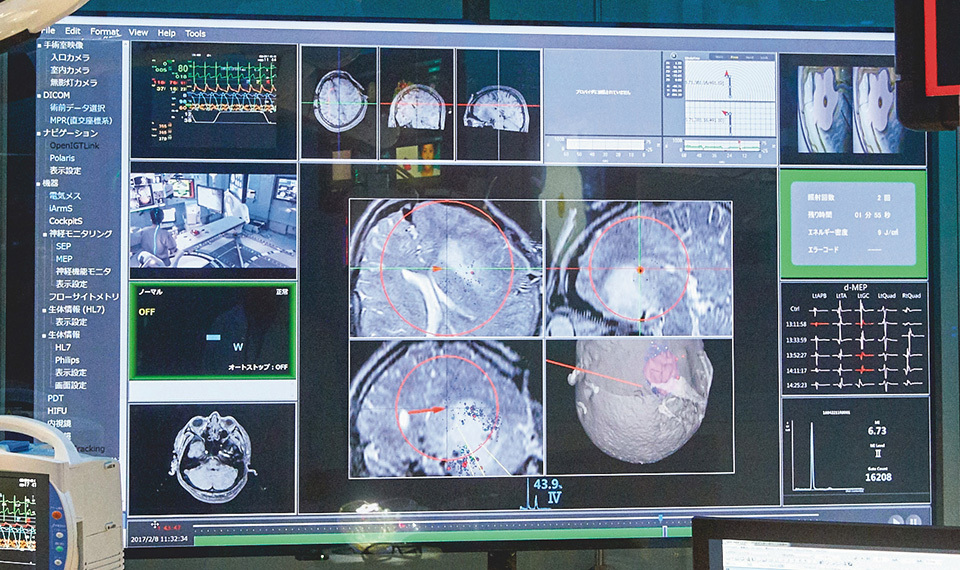
Ultra-high-definition 4K monitors showing comprehensive information from various medical devices within the SCOT theater. The surgery navigation screen, along with the ECG (electrocardiogram) and other physiological data, can be shared with distant medical centers.
MURAGAKI Yoshihiro, professor at the Institute of Advanced Biomedical Engineering and Science at Tokyo Women’s Medical University, explains the significance of the breakthrough.
“Until now, operating theaters have been full of equipment working independently of each other, and data obtained from monitoring the patient, images of the surgical field, and the operating condition of the devices have been displayed without reference to each other, but with SCOT, all the data generated during surgery are synchronized on the same time axis. The data can then be shared over a network in real time with a surgical strategy desk, enabling diagnosis by third parties. The system accommodates telemedicine, allowing even a relatively inexperienced physician to perform advanced surgical procedures under the guidance of a fully-experienced physician.”
The platform for connecting all the devices is the OPeLiNK® interface, sometimes called the “brains” of SCOT. The core technology of OPeLiNK is ORiN (Open Resource interface for the Network), which is industrial middleware that is now being used in smart factories around the world. The driving forces behind the development of SCOT were DENSO Corporation, a well-known Japanese automotive components manufacturer, and Professor Muragaki’s team. OKAMOTO Jun, a Ph.D. in engineering who is part of the team, says, “Surgical navigation is like an automotive navigation system because it shows the exact location of the body being operated on. But it also acts like a flight recorder on an airplane, keeping a record of all the details, such as the path of an electrical cautery knife used by the surgeon, and showing that on the screen, so that everything can be accurately verified during and after the operation. Information that was previously known only to the veteran surgeons is converted into data that other doctors can access.”

Professor of Advanced Techno-surgery MURAGAKI Yoshihiro (right) of the Institute of Advanced Biomedical Engineering and Science and OKAMOTO Jun (left), a specially-appointed instructor in the same field, both at Tokyo Women’s Medical University. Professor Muragaki, director of the Medical AI Center, is an authority on neurosurgery and a world leader in advanced medical science. Okamoto is a developer of iArmS, a surgical robot.
Another member of the development group, DENSO’s OKUDA Hideki, describes how the company, an automotive firm, approached the field of leading-edge medicine.
“In the automotive business, safety and human lives matter more than anything else. Accordingly, the Japanese automobile manufacturing sector, with its overriding concern for safety and reliability, is already suited to designing medical solutions that save human lives. The automotive industry is already expanding its concept of an automobile from just a mobility device to a service that utilizes applications. Medicine is part of that—the age is coming where new values are created by introducing the IoT.”
In October 2019, Okuda and others led the establishment of OPExPARK Inc., a start-up established to accelerate the commercialization of the technology. The first phase of its business involves the launch of an online surgical training service that provides data collected with SCOT to surgeons worldwide. Over 2,000 people have already signed up, mostly neurosurgeons in emerging countries. With surgeons applying SCOT data to their studies, we are entering an era distinguished by a more sophisticated level of medical care.
Now that it is equipped with OPeLiNK, the most practical platform in the world, the day is not far off when SCOT will become one of the primary tools used in operating rooms in hospitals worldwide.

Dr. OKUDA Hideki is executive vice president and founder of OPExPARK, and project general manager of the Social Solution Business Development Division at DENSO. He is involved in researching robotics for medical applications. In addition to his involvement with the SCOT development team, he earned a Ph.D. in medicine from the graduate school at Tokyo Women’s Medical University.
*SCOT® is a registered trademark of Tokyo Women’s Medical University.
*OPeLiNK® is a registered trademark of OPExPARK.