Professor Yamanaka was awarded the Nobel Prize in Physiology or Medicine in 2012, just six years after he had announced generation of iPS cells. This unusually quick recognition bespeaks the impact and sense of expectation produced by iPS cells.
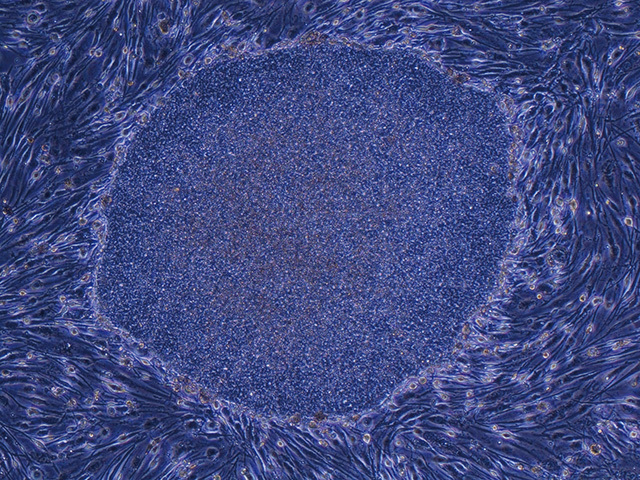
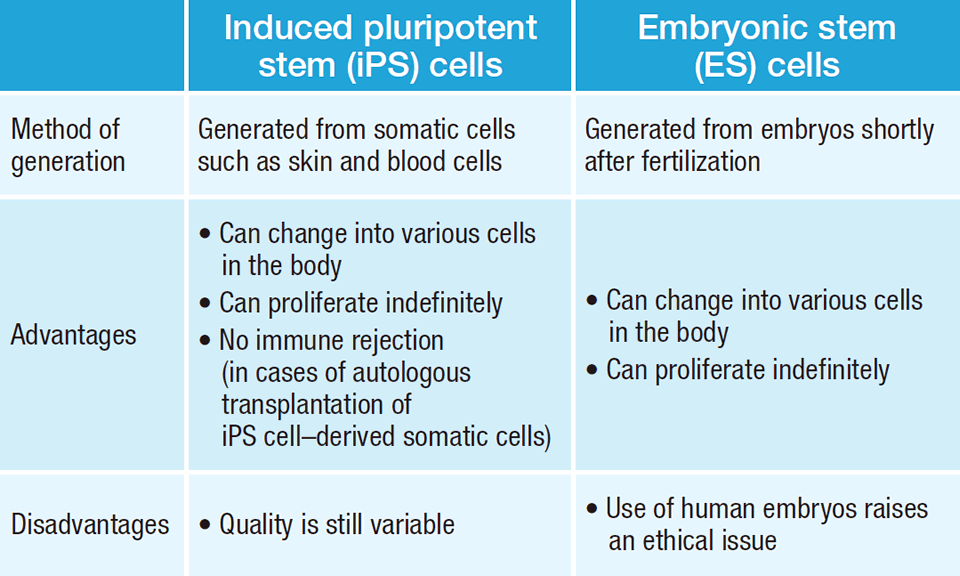
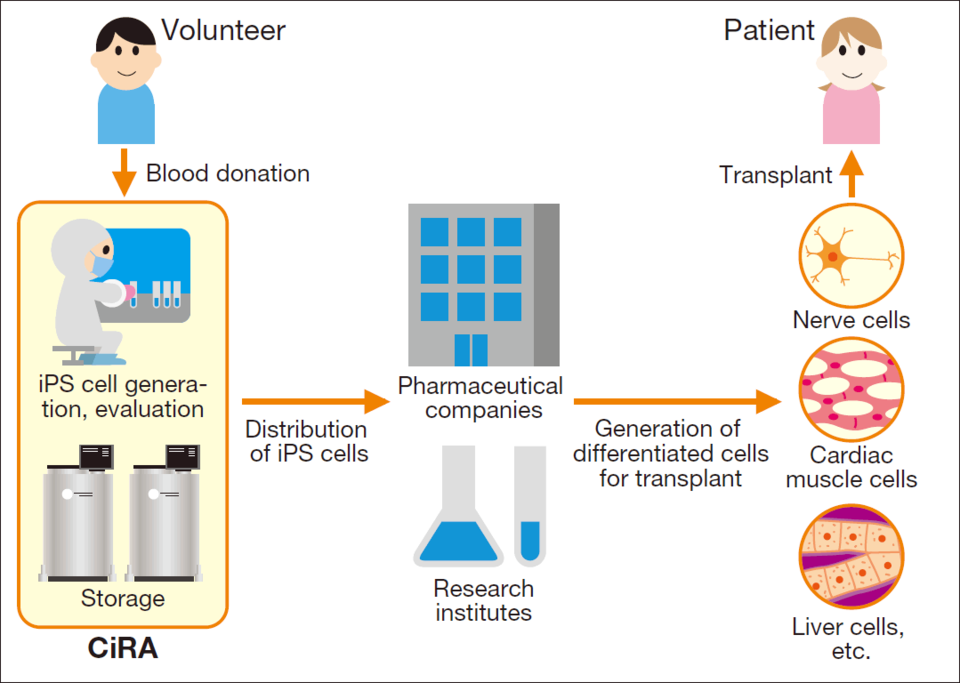
Regenerative medicine uses transplants of cells or tissues to improve the working of organs or tissues that have been lost or become dysfunctional. One of the keys in this endeavor has been induced pluripotent stem (iPS) cells, which have the capacity to change, or differentiate, into various cells in the body. Professor Shinya Yamanaka was the first to announce the generation of such cells in 2006, and in 2012 he was awarded the Nobel Prize in Physiology or Medicine for this accomplishment. Since that time he has continued efforts to develop and spread research in regenerative medicine and drug discovery using iPS cells, working to lower the risks, production time, and costs associated with these cells.
The Center for iPS Cell Research and Application (CiRA) at Kyoto University, where Professor Yamanaka serves as director, was established in 2010 as the world’s first research institute specializing in iPS cells. It is characterized by an open lab style and active fundraising activities, and has more than 200 researchers, graduate students, and technicians. As Professor Yamanaka explains: “Research on medical applications of iPS cells in regenerative medicine and drug development requires time in units of decades. One of my jobs here is to establish a system that will allow CiRA to operate stably over the long term and to create an environment that enables researchers to concentrate fully on their research.”